 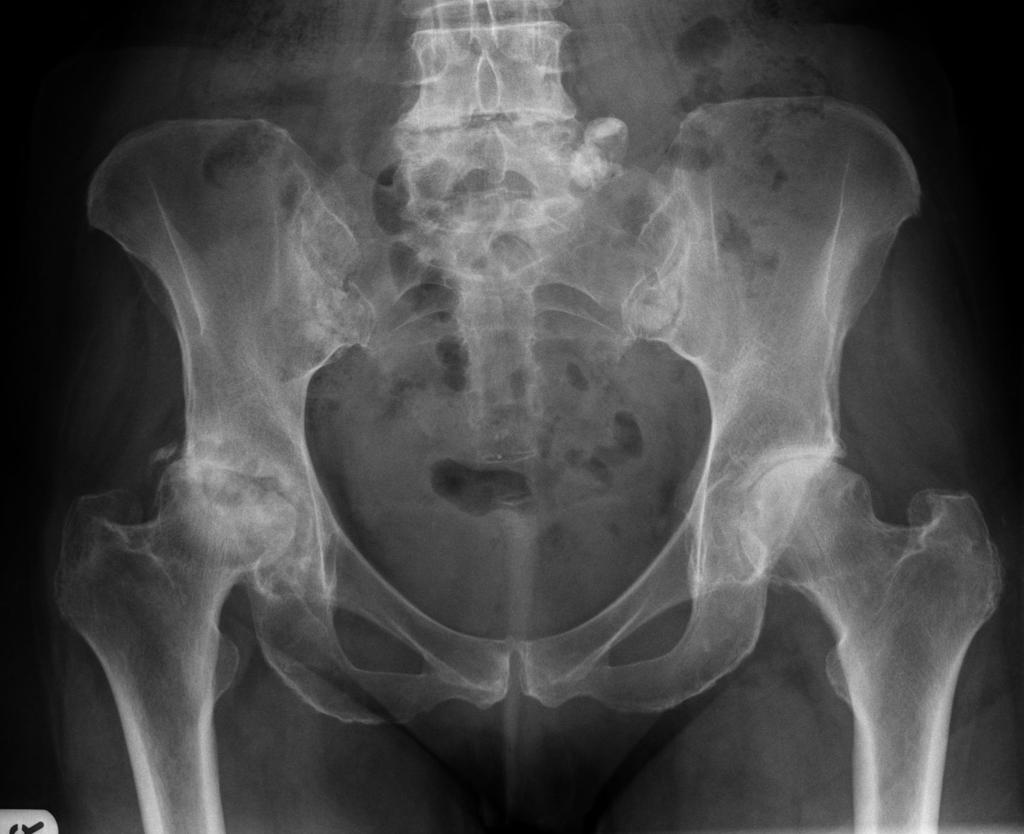
, the direct and associated costs for taking a single postoperative X-ray were estimated from the reimbursement data. The billing data for portable pelvic X-rays were assessed. A random sample of 50 pelvic X-rays was independently reviewed by a second fellowship-trained arthroplasty surgeon. Suboptimal radiographic quality was confirmed based on one or more of the following: (1) malpositioned pelvic X-rays (2) X-rays of incomplete pelvic, bilateral proximal femurs, and implants (3) excessive abduction precluding an accurate assessment of leg length (4) pelvic inlet, outlet, or Judet views due to significant malrotation and (4) the presence of foreign body obscuring relevant anatomical structures. The complications were classified into "known" and "unknown" according to the intraoperative fluoroscopic results recorded in the operative notes. We did not assess leg length, offset, component size, or implant position because the technical parameters were beyond the scope of this study. Complications were defined as hip fractures, dislocations, and fixation failure. Radiographic assessmentĪ fellowship-trained arthroplasty surgeon reviewed all PACU X-rays taken immediately after surgery. The attending surgeons selected the implants. One surgeon used both the direct anterior and posterolateral approaches, and four surgeons used the posterolateral approach. The exclusion criteria included simultaneous bilateral THAs, conversion THAs, THAs due to fractures, revision THAs, and a follow-up period of less than 3 months.Īll operations were performed by 5 high-volume arthroplasty surgeons. The inclusion criteria for the study were (1) patients undergoing THAs through the posterolateral or direct anterior approach and (2) patients taking a standard anteroposterior pelvic X-ray using a portable radiograph machine in the PACU immediately after surgery. The database was queried to identify all patients undergoing THA between Januand December 31, 2018. We retrospectively reviewed the data collected prospectively from our institutional arthroplasty database. We also assessed the quality and cost of the X-rays associated with this protocol. This study aimed to investigate THA complications based on the immediate postoperative X-rays taken in the PACU. argued that immediate postoperative X-rays were not cost-effective because they neither provide additional clinically relevant information nor benefit patient care. They found that 13% of anteroposterior X-rays and 6% of lateral X-rays were inadequate. advocated the use of criteria to determine whether X-rays were adequate. suggested that X-rays were not significantly superior to clinical assessments in diagnosing acute hip dislocations and that no dislocation occurred in clinical practice. Some surgeons often take immediate postoperative X-rays using a portable machine. Immediate postoperative X-rays are often performed in the post-anesthesia care unit (PACU) to screen for complications and assess implant placement, but their effectiveness and cost-effectiveness remain controversial. Periprosthetic fractures and dislocations following total hip arthroplasty (THA) are rare catastrophic complications. The X-rays are often of suboptimal quality, have minimal clinical utility, and are less cost-effective. In total hip arthroplasty, X-rays taken immediately after surgery rarely reveal unknown complications. The cost of a single portable pelvic X-ray was $647. Of the 518 X-rays, 225 (43%) were of suboptimal quality. There was no significant difference between intraoperative fluoroscopy and X-rays ( P > 0.05). Compared to the X-rays taken immediately after surgery, 9 periprosthetic fractures (recorded as "known") were found and 1 was not (recorded as "unknown"). Based on intraoperative fluoroscopy, periprosthetic fractures were found in 10 (2%) THAs. ResultsĪ total of 518 total hip arthroplasties were included in this study. The complications were categorized as "known" and "unknown" according to the intraoperative fluoroscopic results. The quality and cost of X-ray were assessed. 
Immediate postoperative X-rays were reviewed to identify the complications such as periprosthetic fractures, dislocation, and fixation failure. The institutional database was queried to identify all patients who underwent total hip arthroplasty in a single institution between January 1, 2018, and December 31, 2018. The overall quality and cost of X-rays were assessed. This study aimed to investigate the complications of primary total hip arthroplasty based on immediate postoperative X-rays. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
